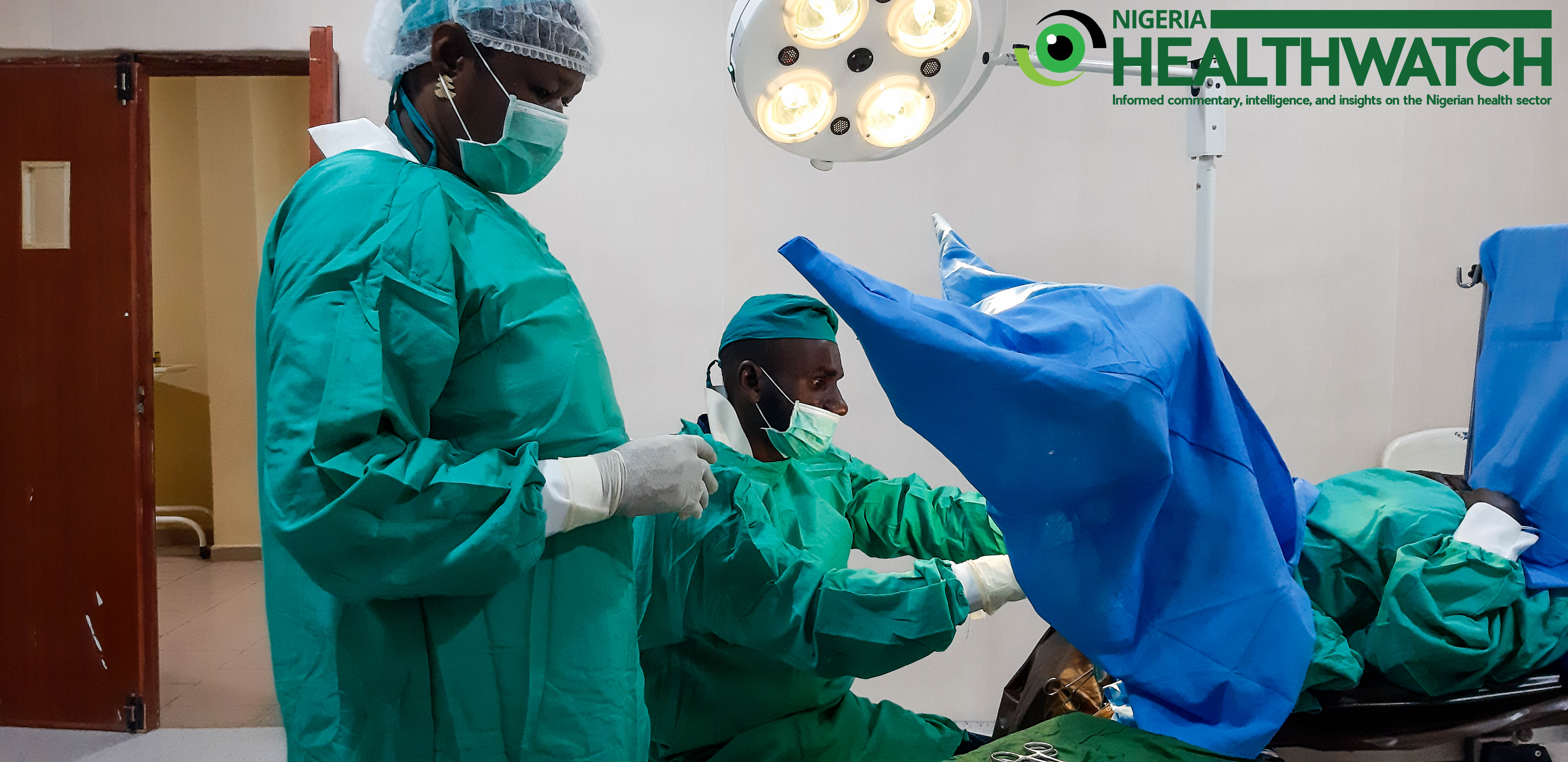
Gesse Vesico Vagina Fistula (VVF) Centre in Birnin-Kebbi is the only facility in the entire state of Kebbi providing care for women suffering from fistula. It has served as a referral centre for VVF since 2005. Today, Dr. Abubakar Dakingari, the head of the centre and his team are performing a routine fistula repair surgery.
Dr. Dakingari takes a moment to catch his breath in between surgeries. “This is what we do every Tuesday, Wednesday and Thursday. We perform surgeries for 200 to 400 women every year,” he says, wiping his brows.
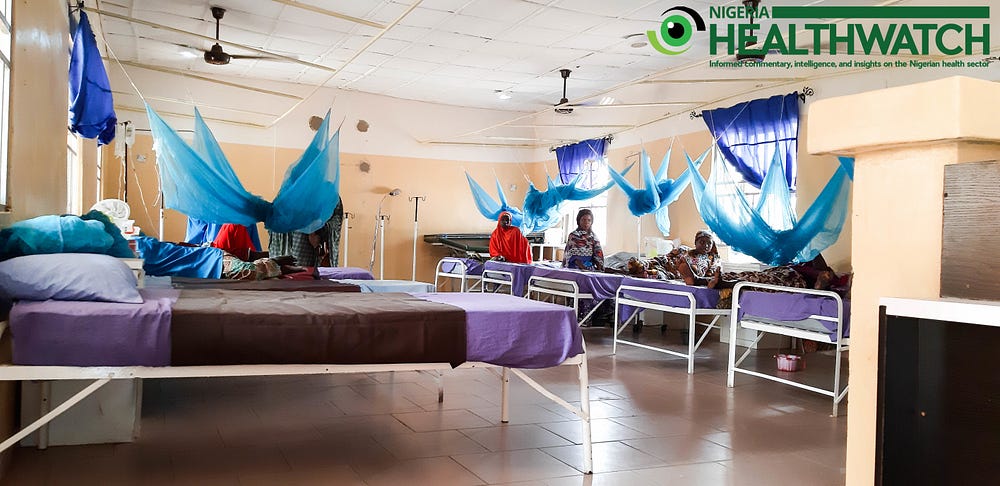
In a nearby block about 10 women recuperate in the post-operative ward after their surgeries. Outside, other women waiting for surgery take refuge from the heat under the many verandas in the hospital. The hospital also has provision for relatives of patients to stay. Designated cooks prepare lunch for the women recuperating and those awaiting surgery.

Another section houses the Family Planning unit, where different methods of contraception are offered to the women before they are discharged. It is a ‘one stop shop’, as women affected by fistula are taken care of from the moment they are admitted to when they are discharged.
Known scientifically as Vesicovagina Fistula or Obstetric Fistula, VVF hinders a woman’s ability to control urination as a result of tissue damage around the vagina and bladder. Causes include factors such as female genital mutilation (FGM) or sexual violence, however the majority of fistula cases are due to prolonged obstructed labour, which is when labour lasts for many hours or days. In an unequal world, women with fistula are the most unequal among the unequal. Many women have lost their homes and their livelihoods, have been kicked out by their husbands and shunned because of the smell of the urine constantly leaking from their vagina.

According to the World Health Organisation (WHO), more than two million women are affected by fistula worldwide, and between 50,000 to 100,000 new cases are recorded every year. Of that number, 40% occur in Nigeria, a worrying statistic in light of the country’s poor maternal health indices. Fistula disproportionately affects women from lower socioeconomic backgrounds, according to Dr. Dakingari, and poor access to healthcare for women before and during childbirth. This is worsened by inadequate and non-functional healthcare centres, and harmful cultural beliefs, the biggest contributors to the rising numbers of fistula patients in Nigeria.

A silent complex problem
Access to healthcare, including standard, well equipped and adequately staffed centres especially at the rural level continues to be a big challenge in Nigeria and contributes significantly to low antenatal attendance and hospital delivery by women. The problem is further compounded by cultural sensitivities prominent in Northern Nigeria, where a large percentage of women neither attend antenatal nor deliver in the hospital.
Married at 16, Umaima Abu, now 18 years old, never attended antenatal care throughout her pregnancy, even though there was a primary health centre in their community, the village of Danga. She says her husband did not grant consent for her to attend. The primary health centre was not always open so when it came time to give birth, she spent close to 24 hours in labour, and was only taken to a hospital in a nearby town of Koko when she became unconscious. “When we got to the hospital; the baby had already died. I had no idea what really happened”, an emotional Umaima says in Hausa.
Umaima thought her ordeal was over after going through a caesarean section to remove her dead baby, only to realise afterwards that she could no longer control her urine. She was referred to Gesse VVF Centre and after living for eight months with the condition, she was recently contacted to come for her surgery, which she was about to undergo.

Bilkisu Ibrahim, 35, just had her surgery and was recuperating in the post-operative ward. The mother of four, who has had three stillbirths in the past, attended antenatal throughout her pregnancy. But despite living in Jega, the second biggest town in the state, with numerous healthcare centres and only 35km from the Federal Medical Centre Birnin-Kebbi, Bilkisu spent over 48 hours in labour, because she “just wanted to deliver at home,” she says.
That did not happen and she ended up having a caesarean section at the Federal Medical Centre to remove her baby, who had already died. She was left with the gripping pain of losing her baby and another unexpected ordeal to contend with; Fistula. She had to live with this life-altering condition for nine months before undergoing surgery. After her surgery, Bilkisu now hopes to return to her community and create awareness about hospital delivery among women using the knowledge she acquired from counsellors at the VVF Centre, so that more women would not make the same mistake she made.
Rehabilitation and livelihood support are critical
According to Dakingari, providing counselling to women affected by fistula goes a long way in restoring their self-esteem. To this end, Kebbi State Ministry of Women Affairs, a co-owner of the hospital, provides counselling sessions for all women admitted to the hospital and builds their capacity with skills like tailoring and bead making. The Ministry also provides a start-up grant and equipment for patients as they are discharged. “The whole aim is to make them self-sustainable when they return to their communities,” says Ministry Permanent Secretary Hajiya Hassana Warra. Dakingari says however that he started getting reports that some husbands would take the equipment from their wives and sell them off to raise funds for the family.

The hospital was getting frequent reports of fistula happening again after women went back to their communities, because they would get pregnant again before they were fully healed. As a result, in 2013, the hospital introduced a strategy of following up with women who have been discharged through phone calls, and now requests that they go to live with their parents or relatives for six months after the surgery instead of going back to their husbands houses immediately. The women are also requested to come to the hospital with their husbands every two months during the period for check-up and counselling. This has greatly reduced the reports of fistula reoccurring among the women.
The Federal Ministry of Health estimated in its 2012 National Strategic Framework for Fistula Elimination that between 400,000 to 800,000 Nigerian women are living with Fistula. There are a total of 11 fistula referral centres in Nigeria like Gesse, including three directly overseen by the Federal Government in Bauchi, Ebonyi and Katsina. These help provide care for about 4,000 VVF patients every year, according to the Strategic Framework.
Still, in total these facilities provide care for barely 0.5% of women living with VVF and other fistula related diseases and it clearly shows that more action needs to be geared towards preventing the condition. The capacity of health institutions at various levels must be improved to provide the care fistula patients need to complement the work of the referral centres.
Nigeria’s Minister of Health, Prof. Isaac Adewole in February 2019, inaugurated a committee on the establishment of more fistula referral centres in the country. This is a step in the right direction, but a collaborative approach must be taken by federal, state and local governments to prevent women from developing fistula in the first place.
WHO’s Guideline for Clinical Management and Programme Development on fistula identified health promotion and awareness creation at the community level as well as provision of comprehensive and quality maternal health services as critical strategies in preventing Fistula. These can be achieved by strengthening the primary healthcare system in the country to provide quality and affordable services at the grassroots, which will help to attract women to the facilities for maternal health services.
Community and religious leaders must help create awareness through health promotion drives, leveraging on their highly respected positions in their communities. They, working alongside centres like Gesse, can help ensure that women like Umaima and Bilkisu have the knowledge of and the access to healthcare centres close to them when they are ready to give birth.


VVF is a sign of non availability of good obstetric care and late identification of pregnancy and delivery danger signs, as well as socio economic challenges of women/families failing to afford health care. In many of these cases where women say they don’t have permission from their husbands, it is as husbands or care givers in families are often afraid of the costs of health care and as such fail to approve in advance the use of health facilities for care, or the health facilities themselves are not welcoming. The NPHCDA new initiative using CHIPS or Village Health workers as is done in some states such as Gombe state is a strategy that can address this.