By Chinonso Kenneth (Lead Writer)
In September 2022, Dr Nnaemeka Alo encountered a critical case at Saint Sabina Catholic Hospital in Agege, Lagos, Nigeria. His patient was a one-week-old baby who was suffering from severe bronchial pneumonia, which significantly reduced her lung function, leading to breathing difficulties and a persistent cough. In addition, the baby was experiencing low blood sugar levels and was nearly unconscious. “The baby needed an ambulance with oxygen for safe transfer to a comprehensive care facility which was a teaching hospital in this case,” Dr Alo explained.
He conducted a Google search for an ambulance service to transport the patient to the Lagos University Teaching Hospital (LUTH) to receive specialised medical attention. “I was not so confident when I got Emergency Response Africa’s (ERA) number from Google. I just tried my luck because this is Nigeria. I called them, and we made a cash deposit. Their response time was less than 45 minutes. Their ambulance came with a nurse and oxygen. The nurse brought the oxygen from the ambulance into the ward so we could commence oxygen on the baby. Immediately we did that, the baby’s colour changed back to pink.”

The patient was eventually transported to LUTH by ERA, where specialists took over the baby’s management.
It was a different experience for Ogene’s pregnant cousin in 2021. “She was rushed to Ikem General Hospital in Isi-Uzo, Enugu State, in a commercial bus, but the hospital had no oxygen and couldn’t do anything, so they referred her to Parklane Hospital Enugu. The same bus was used to transport her again because the hospital had no ambulance. She and her unborn baby died on the way to Parklane Hospital,” he narrated.
ERA: Connecting patients to medical first responders
Emergency Response Africa co-founder, Mrs Folake Owodunni, was inspired to establish the initiative based on personal experience. In 2017, her one-year-old son woke up in the middle of the night, screaming in pain. “Because we were outside Nigeria, I called 911 (an emergency telephone number). The medical dispatcher asked a series of questions and dispatched a response team who arrived at the house and checked him. They realised it was a relatively minor issue, and within 30 minutes of the whole incident, he was asleep,” Owodunni said.
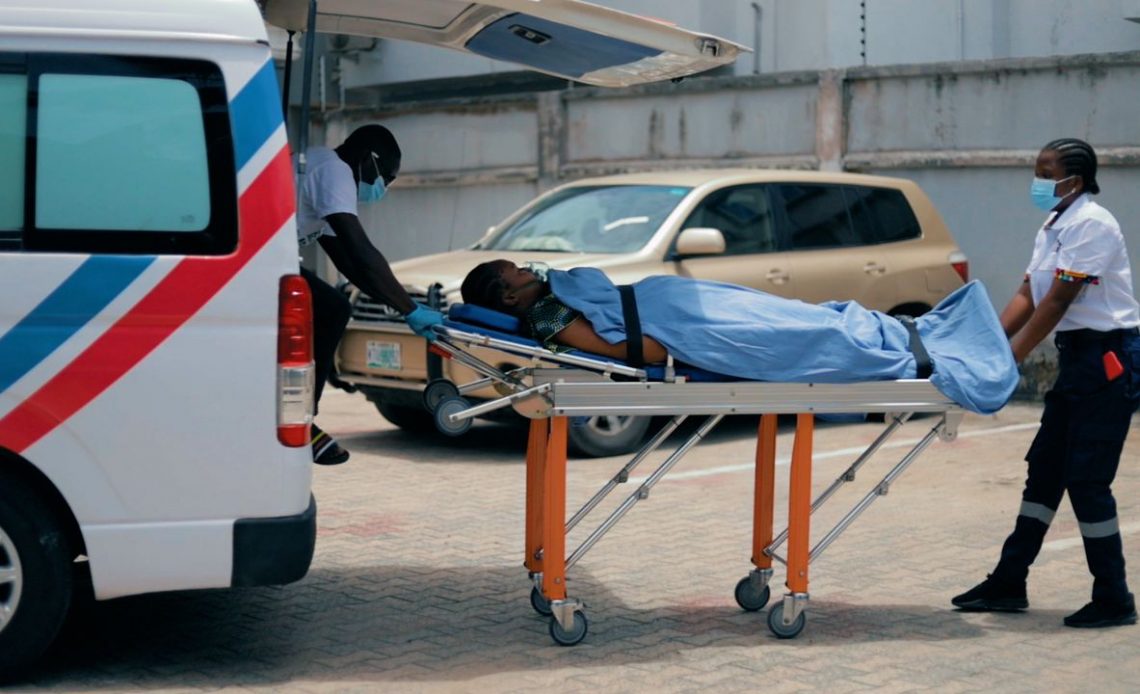
Emergency Response Africa was launched in 2021 with the aim of providing holistic end-to-end prehospital care by connecting patients to a network of medical first responders, emergency vehicles, and verified emergency-ready hospitals in Nigeria, so they can get the help they need in time.
A 24-hour command centre coordinates requests from the ERA toll-free number and mobile app. When a subscriber or one-off user calls the toll-free number or submits a request via the app, the case is connected to either a medical first responder who deploys telephone first aid service to stabilise the patient or an ambulance is dispatched to the location for immediate medical attention and transportation to a health facility, if necessary.
ERA first responders are trained paramedics who stabilise patients during an emergency and facilitate their transport to “an emergency-ready hospital”. That is, a hospital that has bedspace to accommodate the patient, oxygen (if the patient needs it) as well as a doctor on hand to attend to the patient. To determine if a hospital is emergency ready, ERA staff calls one of the already verified 82 emergency-ready hospitals in their network. These hospitals are distributed across Abuja, Lagos State, as well as the cities of Ibadan, Port Harcourt, Warri, and Enugu, where they are active.
In addition to their ambulance response team, ERA also employs a motorcycle medic unit that uses motorcycles to provide faster first aid and emergency response in situations where rapid intervention is crucial.
Dr Alo noted that while using ERA’s service for the second time in April 2023 — after a 34-year-old female patient underwent surgery for severe preeclampsia and became unconscious — the nurse attached to the ERA ambulance introduced him to the idea of identifying emergency-ready hospitals or those with ‘bed space’ before transporting a patient there.
“Initially we wanted to go to the teaching hospital, but the ERA nurse was of the opinion that the teaching hospital might not have bed space this time, and it’s better we confirm first. When we called, there was no space, and she had to make calls to other hospitals. Eventually, we got Genesis Hospital and transferred the patient there,” Dr Alo said.
A basic annual subscription plan at ERA sells at N35,000 per person. This gives them access to emergency motorcycle and ambulance services and an accident insurance product to give additional financial cover. One-off users pay above N50,000 for a single medical emergency response. If a person cannot pay the one-off fee, ERA can either provide phone first aid or refer them to government agencies that can assist.
“We have connected a network of first responders, ambulances and hospitals using technology such that if someone requires help, they reach out to us, and we can dispatch the closest available response team and then transfer them to hospitals as needed,” Owodunni said.

“Most people still believe ambulances are for transporting corpses”
Data from ERA indicates that they have received a total of 1,243 medical emergency calls, with one out of every four calls resulting in transportation to a hospital. However, poor road infrastructure as well as traffic congestion have been a challenge. Owodunni also expressed concern over the limited awareness and understanding of emergency services in Nigeria. Most people still believe ambulances are for transporting corpses. “Paramedicine as a field is not widely known in Nigeria, therefore, the pool of people who understand what it means to deliver emergency medical services in Nigeria is limited,” she added.
The impact of the medical brain drain is also a challenge as ERA must constantly replenish its talent pool. Owodunni revealed that three of her most experienced staff resigned this year because they were relocating abroad.
Emergency response in Nigeria
Emergency response in Nigeria is grossly inadequate. Data from the National Emergency Medical Services and Ambulance System (NEMSAS), which is yet to fully take off, reveals that the lack of adequate Emergency Medical Services (EMS) in Nigeria contributes to up to 50 per cent of maternal, neonatal, and infant — as well as road traffic accident — morbidity and mortality rates.

Nigeria has faced significant challenges in establishing a robust and effective emergency medical service and ambulance system. In 2016, an Emergency Medical Services (EMS) policy was developed to coordinate and integrate emergency medical services in Nigeria. In a bid to boost emergency response, in 2022, the Federal Ministry of Health launched the National Emergency Medical Service and Ambulance System (NEMSAS) to provide urgent health service to Nigerians at the point of distress, with no cost at the point of care, within the first 48 hours. However, there have been no subsequent reports regarding the initiative’s activities or progress.

Emergency Medical Service and Ambulance Systems are critical components of a well-functioning healthcare system. In emergencies, quick access to medical care can significantly improve survival rates and reduce the severity of injuries or illnesses. Public-private partnerships (PPPs) can play a significant role by leveraging the strengths and resources of both sectors. According to Owodunni, ERA’s plans include partnering with state governments to institutionalise emergency medical services across states.
There is clearly an urgent need for an effective state-wide and country-wide emergency medical service in Nigeria. There is no doubt that until then, many avoidable deaths will continue to occur, we can and must do better. “The Nigerian patient is worth it”.