Chris Bassey and Hannah Ajayi (Lead writers)
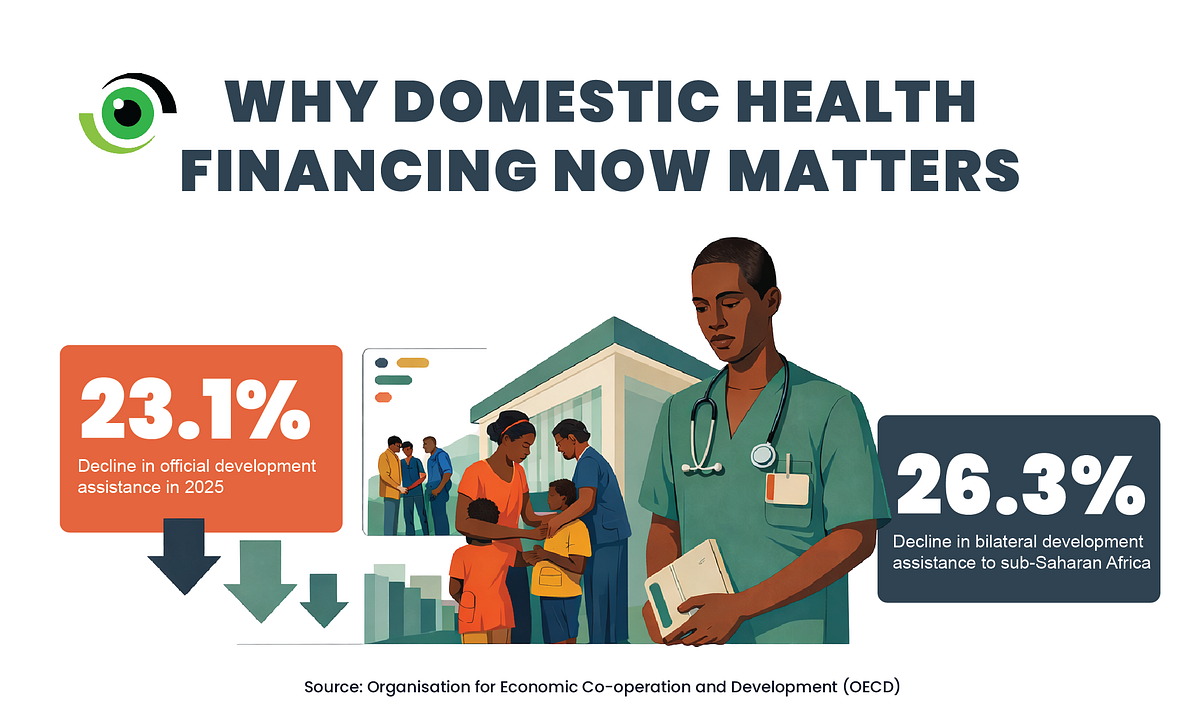
As official development assistance (ODA) continues to decline, governments are coming under growing pressure to mobilise domestic resources to fund healthcare. Preliminary data show that official development assistance (ODA) declined by 23.1% in 2025, marking the largest annual drop on record, while bilateral ODA to sub-Saharan Africa fell by 26.3%. Essentially, this forces countries to confront the challenging question of how to fund health more sustainably, as external support becomes less predictable and domestic needs continue to grow.
The World Health Organization (WHO) has made it clear that progress towards universal health coverage (UHC) will depend on how countries strengthen public revenue for health. As such, attention is increasingly turning to fiscal measures that can improve population health and expand health funding. The use of health taxes has re-emerged on the global agenda as a practical policy lever.
Through its 3 by 35initiative, WHO is encouraging countries to implement well-designed taxes on tobacco, alcohol, and sugary drinks to reduce harmful consumption, while generating revenue, estimating that these policies could generate an additional US$1 trillion globally over the next decade.
In Nigeria, this shift is beginning to take shape through ongoing discussion around sugar-sweetened beverages. The current excise duty, introduced under the Finance Act 2021, set a rate of ₦10 per litre in 2022. Policymakers are now considering how that structure might be revised. At this point, the question is no longer whether health taxes should form part of the policy conversation. It is whether the health taxes can be designed in a way that is robust enough to deliver meaningful health and revenue gains,
In an interview with Nigeria Health Watch, Dr Mary-Ann Etiebet, President and CEO of Vital Strategies, noted that health taxes are gaining prominence because they sit at the intersection of two pressing priorities; reducing the burden of preventable disease and strengthening more sustainable domestic financing for health.
Health taxes as a strategic policy tool
For Dr Etiebet, countries that take health taxes seriously are doing more than just adding a fiscal tool to their policy options. They are making a strategic decision about the type of health system they want to build and the broader direction of their economies. “These are countries that are not only setting their health agenda for the future,” she explained, “they are also setting their economic agenda.”
Too often, health taxes are framed narrowly as revenue-raising measures or as tools to discourage unhealthy behaviour. In practice, their role is more structural. They operate at the intersection of three pressures governments can no longer treat separately, preventing avoidable diseases, reducing long-term treatment costs, and securing more reliable domestic financing for health. WHO now describe well-designed health taxes as “win-win-win” policies because they save lives, generate revenue, and can promote health equity when implemented effectively.
Nigeria’s context makes this argument difficult to ignore. According to the World Bank, drawing on WHO data, out-of-pocket payments account for 71.9% of current health expenditure in the country. In such a setting, prevention cannot be treated as a secondary concern. It is part of the funding challenge. A country cannot keep asking households to absorb both the cost of illness and the gaps in public funding risks deepening inequality over time.
Why poorly designed health taxes fail to deliver impact
One of the central points in Dr Etiebet’s argument is that not all health taxes deliver meaningful results. Some taxes serve mainly as indicators. They generate attention, often meet resistance, and then underperform because rates are too low or the design is too weak to shift behaviour. “If health taxes are not designed well, they risk quietly eroding a few years after adoption,” she said.

That warning is particularly relevant currently. WHO’s health tax guidance makes clear that the effectiveness of health taxes depends on their ability to make harmful products less affordable over time. This requires tax increases to be large enough to outpace both economic growth and inflation in real terms. WHO also emphasises that excise taxes are the most effective approach to health promotion, especially when structured around quantity or harmful ingredients, such as sugar, rather than solely on product value.
The WHO’s 2025 global report on sugar-sweetened beverage taxes shows that at least 116 countries now levy taxes on sugary drinks. That matters not because policies should be replicated wholesale, but because it shows that the question is no longer whether such taxes are politically imaginable. It is whether governments are willing to adopt designs that deliver measurable health and revenue gains. The WHO’s broader health-tax initiative also highlights that nearly 140 countries raised tobacco taxes between 2012 and 2022, showing that significant change is achievable when governments concentrate on policy design and implementation.
For Nigeria, this should sharpen the policy test. If the goal is genuinely to cut sugar consumption and expand fiscal space for health, then the country must go beyond simply announcing a levy. It needs to consider how the tax performs over time, whether it remains effective in real terms, if it incentivises reformulation, and whether it is administratively robust enough to resist dilution. That is what differentiates a tax that merely exists from one that truly works.
Trust, fairness and political durability
Even a well-designed tax can fail if the public perceives it as another government-imposed burden without a clear justification. As Dr Etiebet noted, “When people hear the word ‘tax’, they think something is being taken away from them.”

This is not simply a communication challenge, but it goes to the heart of political stability. Health taxes are more likely to endure not only because they are technically sound, but also because they are clearly explained and linked to outcomes that people can understand and relate to.
The WHO’s current analysis suggests that the overall effect of health taxes can be progressive if governments account for how health benefits and costs are distributed, including reductions in preventable illnesses, income losses averted and declines in catastrophic health spending. This is especially relevant in Nigeria, where households already carry a significant share of health expenditure.
The test for Nigeria’s health financing choices
Nigeria’s sugar tax debate is about more than beverages or incremental revenue. It reflects a broader question of whether the country is prepared to approach health financing with greater discipline and ambition. In a period of tighter aid, health taxes should be held to a higher standard. Are they designed strongly enough, applied fairly enough, and communicated clearly enough to influence both behaviour and the wider financing landscape?
If Nigeria can address that question directly and take meaningful action, then the current debate on health tax could move beyond a narrow focus on sugary drinks. It could serve as an example of how a deliberate shift towards financing a greater share of the country’s health needs domestically could have beneficial implications for both equity and long-term health system resilience.