By Rabson Kondowe (Lead Writer)
Clara still vividly remembers the day in 2019 she felt unwell while at school.
“I was in Mathematics class, then all of a sudden my body was very hot, I was sweating and I had a headache. I felt weak,” says the 14-year-old. “I informed my teacher and he took me to a classroom to test me for malaria.”
In the classroom, Clara was handed over to another teacher who tested her for malaria. When Clara’s malaria test came back positive, she was given anti-malarial drugs and sent home to her parents who were told to follow the dosage prescribed by the teacher. Within three days, Clara was well and back to school.

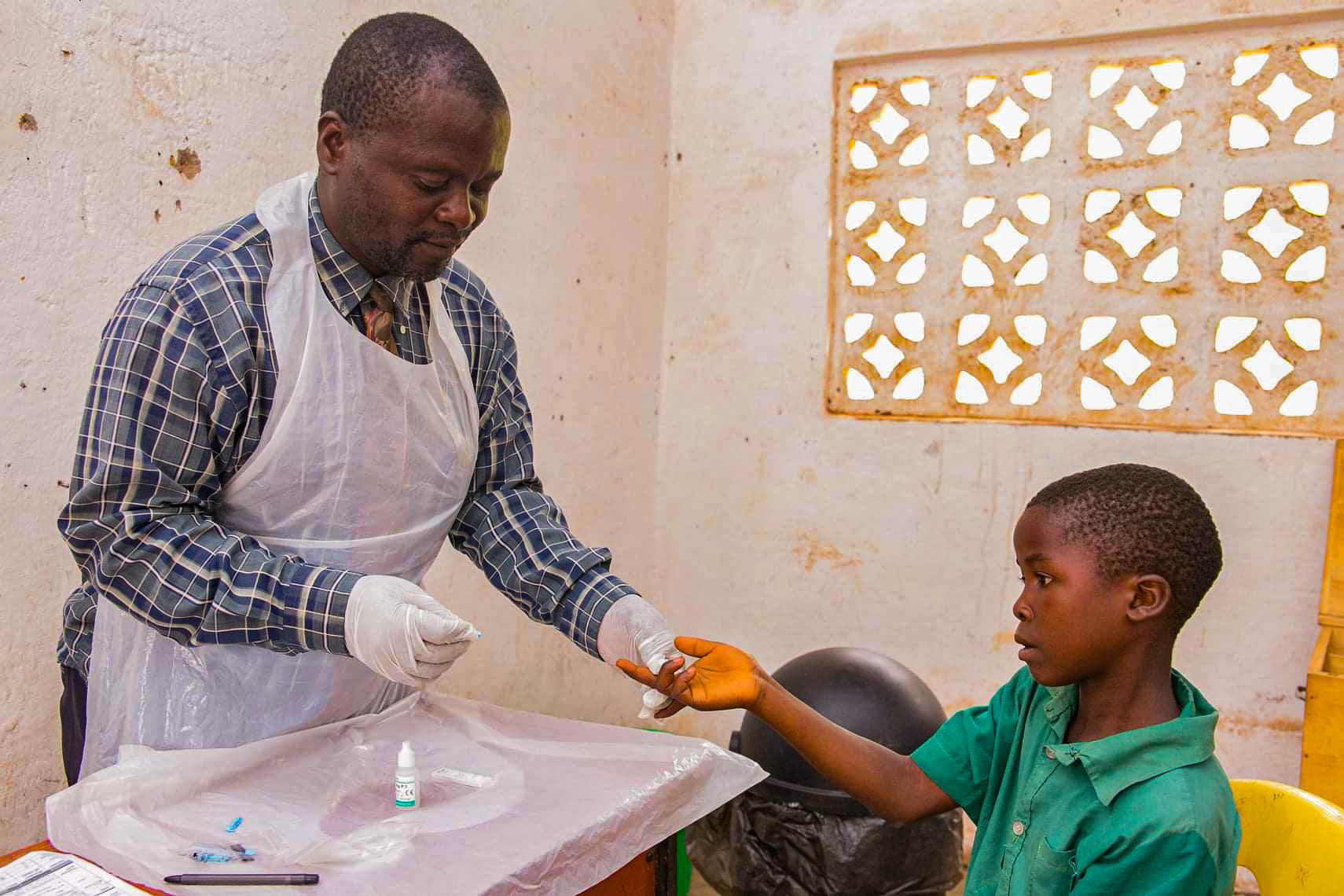
Gologota Primary School in Makupete village is one of 58 public schools in the area of Traditional Authority (T/A) Chikowi in Zomba district, southern Malawi where primary school teachers have been trained to use malaria rapid diagnostic test (RDTs) to identify and treat school children for uncomplicated malaria infections through Learner Treatment Kits (LTK) Initiative. These kits contain rapid diagnostic tests for malaria, antimalarial medicines and other treatments for minor common health problems like headaches, eye infections, and minor wounds.
Save the Children Malawi together with the National Malaria Control Programme (NMCP) of the Ministry of Health implemented the LTK initiative in 2013. It was noted by the implementers that malaria among primary school-age children was a big threat to the health and education of this age group. According to Severe Malaria Observatory, Malawi is among the top 20 countries with the highest malaria prevalence and mortality rates. A study done by the College of Medicine, University of Malawi with the London School of Hygiene and Tropical Medicine, reports that transmission of malaria in Zomba district, is particularly intense, with 60% and 32% of primary school-aged children having malaria parasites and anemia, respectively during the peak malaria transmission season between November and April.

“There’s a high burden of malaria in school going children and we discovered that a lot of pupils go to school while infected with malaria. So, we decided to train the teachers to be able to treat malaria in children right there at the school,” says Gome Jenda, Senior Adviser on Health and Nutrition at Save the Children Malawi.
The 58 schools have a dedicated room where teachers known as LTK dispensers conduct the tests. The LTK is available every day during school hours but the tests are only carried out when the learners feel unwell. When a child tests positive for malaria, he or she is given paracetamol and lumefantrine-artemether commonly referred to as LA, which the children take for three days. LA is the first line of treatment for uncomplicated malaria in Malawi. For serious cases, caregivers of the learners are advised to take their children to local health facilities in the district.
According to Jenda, there is a direct link between the health centres and the schools. “The schools get the drugs and supplies from the health centres through the Ministry of Health. When the supplies run out, the LTK dispensers write a request for more supplies,” he said.
But the LTK is not a programme that is being carried out in a vacuum just at schools. The initiative is working closely with the community through encouraging caregivers to be aware that the intervention is not a replacement for routine health facility-based care but an additional service that could be accessed during school hours. “We constantly tell parents and guardians to know that the school is not a treatment place, we tell them not to allow their child to go to school with a fever, rather take the child to the hospital. LTK is only there to help children when they begin to feel unwell while at school,” Jenda said.

Since children are now able to receive treatment right at school, it means that they do not have to walk with their parents for long distances to go to the nearest clinic, a situation that is common in rural areas in Malawi.
One of the biggest challenges of the programme is adequate resources to test more children. “At the moment we are not operating to a level that we want because of project resources for instance we want train as many teachers as possible but at the moment we are not able to do that,” Jenda said. Secondly, the programme is also facing a shortage of teachers in primary schools due to the nationwide teacher shortage. Malawi has one of the world’s most dramatic teacher shortages, equivalent to 2% of the global teacher posts standing empty. For this reason, Jenda says they are struggling to roll out the programme in other areas in Zomba at the moment.
Ethe Nsanama teaches Agriculture and Social Studies at Gologota Primary School. She is an LTK dispenser who was trained by Save the Children and the Ministry of Health to test and treat children at the school. Nsanama reports that the programme is helping a lot of children at the school especially during the rainy season when malaria is rampant. “During the peak season of malaria, we can test about 20 children in a day”, she said, adding, “Before the programme was introduced, children had to walk with their parents to a local government facility which is six kilometres from Makupete.”
However, Nsanama says even though the school made a duty roster for teachers to carry out the tests, the number of teachers who test and treat the children is small. For instance, Gologota Primary School has 25 teachers in a student population of over 1,500 but only 4 teachers at the school were trained.
Another challenge according to Nsanama is the shortage of drugs that are usually supplied at the school “Since January, we have not been able to treat children because we are out of drugs, we are still waiting for the health centre to supply us,” she said.
According to Save the Children, between March 2019 to February 2020, teachers in the programme have conducted 7,900 tests with 6,101 cases being positive.
Saidi Ndau, the Malaria Coordinator at the District Health Office in Zomba, says the intervention is contributing to the management of malaria cases in Malawi. “The provision of the treatment kit in schools means that we are minimising the work for health workers, this also means that we are minimising the long queues that are usually at the facilities,” he said. To ensure that teachers do not go overboard by treating other serious diseases, Ndau says they are doing regular supervisions at the school.

Since the programme only covers Chikowi area in Zomba, plans are in the pipeline to scale up at the national level. “We want to expand the programme throughout the country because we have seen how imperative it has been. We have been able to pick up a lot of positive cases and we have been able to treat them,” says Dr Michael Kayange, the Manager of National Malaria Control Programme in the Ministry of Health.
The intervention is particularly keen on decreasing the rate of absenteeism in schools. So far, the strategy is working. “A lot of schools have reported that a lot of children return to class immediately when they receive treatment,” says Dr Kayange. As of 2020, the attendance rate was at 88%, he said.
Village Headman of Makupete, Henry Masambuka Makupete, says the village understands the significance of the programme. “A lot of parents and guardians are very appreciative of the LTK because children are now able to receive treatment quickly,” he said. However, Makupete is of the view that the community still needs a well-equipped health facility nearby because the LTK is only available when school is open.
Margret Mwanga from Makupete village is a mother of six. Last year two of her children tested positive for malaria, received treatment and went back to class. “It is a great relief to us, instead of us parents taking the sick learner to the health facility for treatment, we are spared that task,” she said.

In Munyapa, a village near Makupete, John Butao, a father of two, admits he was skeptical about the programme when it first started. “I was not comfortable with the idea of teachers treating children including my own,” he says. But when Butao learned that the teachers were trained to diagnose and treat malaria in children, he began to look at the program in a different light. “I see the goodness of this programme, just last year my first-born son got sick while at school. He got tested and was found with malaria. He was treated at the school and he continued taking medication at home, and on the third day my boy was able to return to school,” he said.
For Clara, the programme has had a surprising side effect on her ambitions. “Whenever I see many of my friends receiving help at the school clinic, I’m always motivated to become a doctor,” she says with a smile on her face, adding, “I want to save lives.”

Can the LTK Initiative be adapted to support Nigeria’s malaria elimination efforts?
Malaria is a major public health problem in Nigeria where it accounts for more cases and deaths than any other country in the world. According to the 2019 World Malaria Report, although the total number of malaria deaths in Nigeria reduced between 2010 and 2018, from almost 153 000 deaths in 2010 to about 95 000 deaths in 2018, Nigeria still had the highest number of global malaria cases (25 % of global malaria cases) in 2018 and accounted for the highest number of deaths (24 % of global malaria deaths).
According to the 2015 Malaria Indicator Survey, malaria prevalence among children under five years of age was 27 % in Nigeria; however, there are significant regional, rural-urban, and socioeconomic differences. School-aged children across the country miss school because they are sick with malaria.
The Federal Government of Nigeria initiated in 2016 the National Home Grown School Feeding & Health Programme (HGSFHP). The vision was to implement a sustainable school feeding programme that will establish a safety net for the poor and eradicate malnutrition in school age children, while stimulating the national agricultural economy. The National Home Grown School Feeding Programme aims to feed 5.5 million primary education students one meal a day for all public primary schools annually. The HGSFHP provides opportunities to assist vulnerable families feed their children while providing an incentive to send them to school.
Can an intervention such as the LTK Initiative be introduced alongside the school feeding programme to help reduce the number of children who miss school as a result of malaria? If teachers can be trained to test children when they fall sick at school with RDTs, treat those who test positive, and provide parents with directions for care, such a programme could complement the nutritional goals of the school feeding programme, keeping Nigerian children healthier overall. However, like the LKT Initiative, to ensure sustainability, stable funding sources would need to be ensured, as well as the required human resources in schools to ensure diagnosis and treatment of children who have malaria.