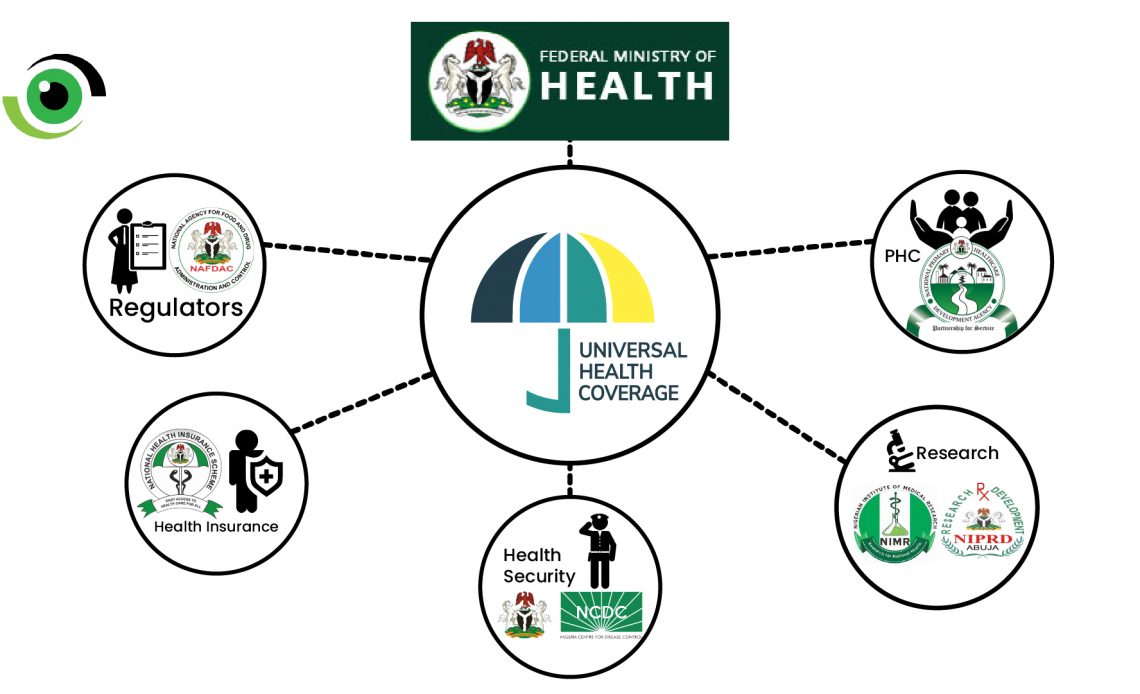
Universal Health Coverage (UHC) is a health-systems performance outcome where people have access to quality health care where and when they need it, without financial hardship. Coverage can be defined in two ways: the range of health services provided (promotive, preventive, curative, rehabilitative, and palliative) and the proportion of the population covered. While no country can provide health services to 100% of its population, measures that ensure that the poorest and most vulnerable are cared for are critical.
UHC2030: Where are we?
The Sustainable Development Goals (SDG) indicators 3.8.1 (coverage of essential health services) and 3.8.2 (catastrophic health spending) are used to track progress towards UHC. According to the 2023 SDG report, progress in health service coverage has significantly slowed, and in 2019, 381 million people (4.9% of the global population) were pushed into extreme poverty due to out-of-pocket health expenditures. This decline in progress is due to several factors, including the COVID-19 pandemic, the war in Ukraine, and economic crises. These factors are unprecedented and underscore the urgent need to invest in building resilient health systems capable of withstanding such shocks.

A 2022 systematic review of factors influencing countries’ progress toward achieving UHC revealed challenges in stewardship, resource creation, financing, and service delivery. Factors related to stewardship include a lack of coordination within the Ministry of Health and managerial inefficiencies in health insurance schemes; those related to resource creation include inequity in allocating public health resources, and those related to financing include inadequate financing, fragmented financial arrangements, and inefficient use of resources. Key recommendations around revenue raising, collection and utilisation, strategic purchasing, and investments in primary healthcare as the bedrock of UHC all point toward one key enabling factor — strengthened government stewardship.

Nigeria launched its National Health Insurance Scheme (NHIS) in 2005, but only passed a law establishing mandatory health insurance in May 2022. According to the 2018 National Demographic and Health Survey (NDHS), the country has only achieved coverage for 3% of the Nigerian population. Most people with health insurance coverage are in the formal sector, and the reasons cited for this low coverage, include poor policy implementation due to a lack of policy awareness, low government spending on health, and poor evidence-informed decision-making, in keeping with global challenges. As a result, Nigeria is far from achieving the SDG 3.8 target of “achieving universal health coverage, financial risk protection, access to quality essential healthcare services and access to safe, effective, quality, and affordable essential medicines and vaccines for all” by 2030.
Politics is key to improving government stewardship for the achievement of UHC
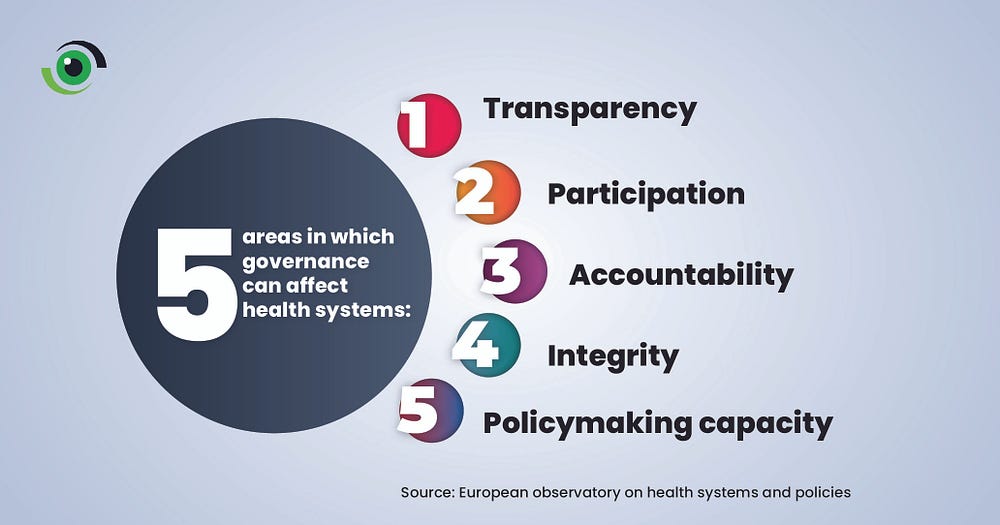
Universal Health Coverage (UHC) is political, and addressing the challenges affecting the achievement of UHC requires an understanding and consideration of the political economy, which drives political will, leadership, and governance. Good governance engenders transparency, accountability, participation, integrity, and improved policymaking ability, collectively resulting in a stronger, more efficient health system.
There is a need to strengthen Nigeria’s political economy for health; the public needs to become more aware of health as essential for their economic growth and prosperity, and thus demand it from politicians, who will then be pushed to prioritise it in their agenda. The weak political economy for UHC in Nigeria is evidenced by persistently low government spending on health, with the federal government having never met the 2001 Abuja Declaration of allocating 15% of its total budget to health. No country has achieved UHC without significant public spending and consistent spending on health service delivery tends to boost political capital — this must be prioritised in Nigerian politics.

In October 2022, Nigeria Health Watch hosted the 8th annual Future of Health Conference, capitalising on the then-upcoming political reset window brought about by the 2023 general elections to put health at the top of the political agenda. The conference’s theme “The Political Economy of Health: Investing in the Future of Nigeria,” centred on the political determinants of health and the interplay between social, political, and economic factors that shape population health outcomes. In discussing the importance of cultivating political will for improved health outcomes, panellists emphasised the need for focused communication with the political class that factors in multiple stakeholders’ interests.
How can health managers, duty-bearers, and civil society organisations secure and sustain political will and support for programmes and initiatives toward achieving UHC? Key recommendations included communicating in clear, simple language to spur citizens’ engagement to demand UHC from the political class and hold them accountable, as well as framing UHC in a language that politicians understand — as an investment for economic growth.
New leadership in the Nigerian health sector tasked with achieving UHC
Following the appointment of the new Coordinating Minister of Health and Social Welfare by the new administration in August 2023, there have been some additional changes in leadership in the Nigerian health sector, including the appointments of new Director Generals (DGs) of the National Health Insurance Authority (NHIA) and the National Primary Health Care Development Agency (NPHCDA), both of which are responsible for expanding health insurance coverage and access to quality primary healthcare. These new leaders will be held accountable for delivering the new administration’s health agenda, which aims to achieve health insurance coverage for at least 40% of the population (50 million Nigerians), mostly poor and vulnerable people, by 2025.
Previous administrations established solid frameworks for this with the National Health Act (2004) and the National Health Insurance Authority (NHIA) Act (2022), which established the Basic Health Care Provision Fund (BHCPF) and the Vulnerable Group Fund respectively, both instruments that aim to ensure coverage of the poor and vulnerable. These laws took many years to pass and required significant political will and energy from both executive and legislative branches of the government. Implementation of the recently launched NHIA operational guidelines will require the same — strong political will and leadership. It is critical that stakeholders — duty bearers, health managers, civil society organisations and the public do not rest on their laurels and continue to push for UHC and keep it elevated at the top of Nigeria’s political agenda.