By Rabson Kondowe (Lead Writer)
In 2020, Maxwell Yambeni encountered a life-threatening situation involving a patient at Chikwawa District Hospital in southern Malawi. A fifteen-year-old girl with a perforated uterus was in a critical state, and her condition was rapidly deteriorating.
“She was in very bad shape, battling severe anaemia and alarmingly low levels of haemoglobin. It was not a simple case,” recalls Yambeni, a clinical associate in general surgery at the hospital. Recognising the severity of the situation, he turned to a WhatsApp group called SURG Africa Managed Clinical Network (MCN) for immediate advice on transferring the patient to Queen Elizabeth Central Hospital in Blantyre, approximately 50 kilometres away.
An experienced surgeon at Queen Elizabeth Central Hospital learnt about the case from the WhatsApp group and proposed an alternative approach which was to guide Yambeni and his team through the surgery remotely before arranging for the patient’s transfer.
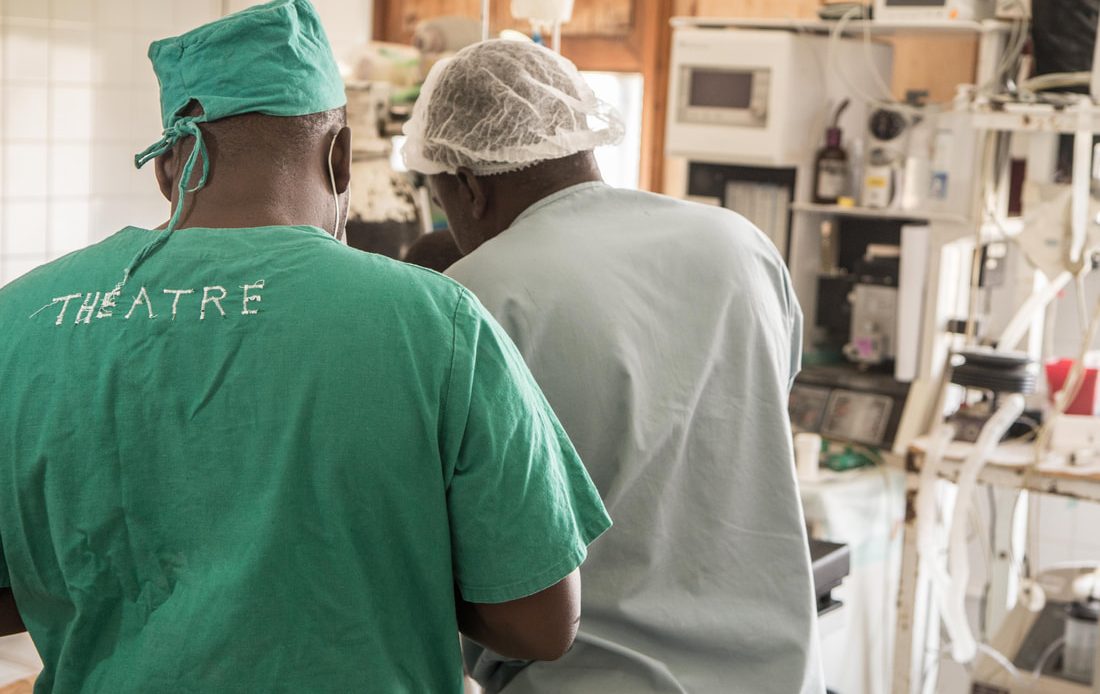
“The patient was in septic shock and needed intensive care immediately after the operation. Here [Chikwawa District Hospital], we have one ventilator which is at the theatre,” said Yambeni, the gravity of the situation still evident in his voice. “We don’t have an ICU here, and after the operation, we used the anaesthetic machine, which interrupted the operation of our theatre for 24 hours which was not safe for other patients as well.”
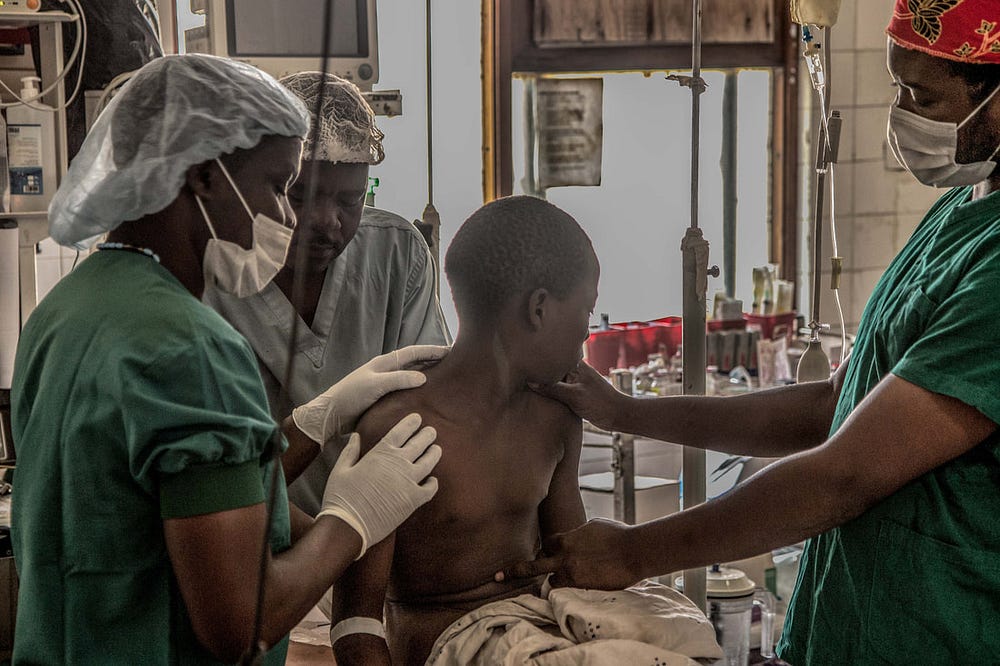
Eventually, Yambeni was courageous enough to successfully operate on the young girl. The girl was later transferred to Queen Elizabeth Central Hospital. “Today, she’s alive and well,” he said.
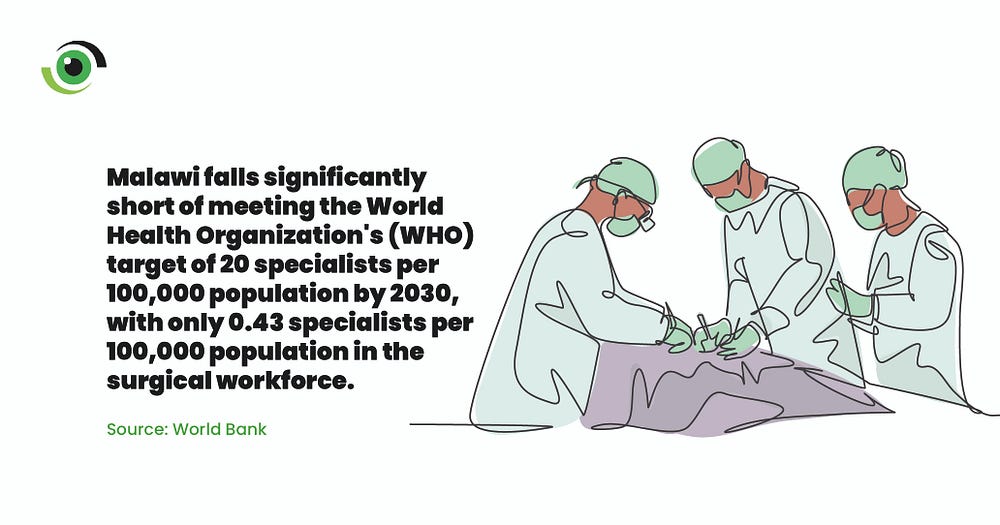
A 2020 study by the World Journal of Surgery on access to surgery in Malawi revealed that there is a shortage of fully trained surgeons, anaesthetists and obstetricians in district and rural hospitals, posing a significant challenge to health care in a country where 84% of the population lives in rural areas. The country’s specialist surgical workforce is 0.43 per 100,000 population, according to the World Bank, this is far below the Lancet Commission on Global Surgery recommended target of 20 per every 100,000 population by 2030.
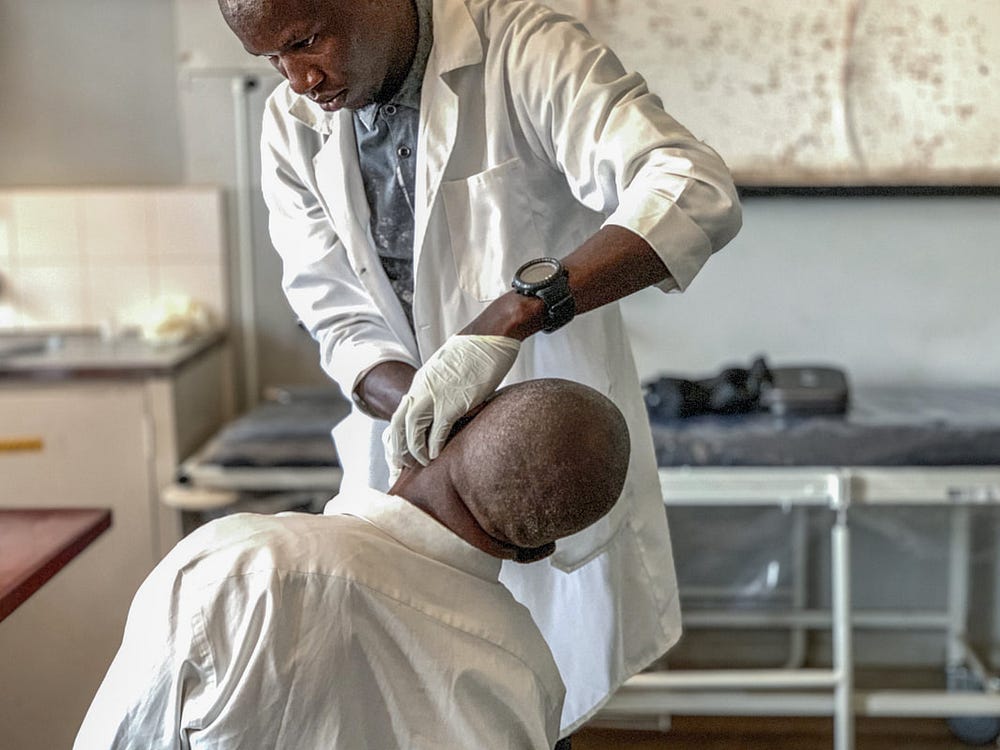
Health specialists in Malawi are mostly found in the four tertiary hospitals located in Blantyre, Lilongwe, Zomba and Mzuzu. As a result, rural hospitals rely on clinical officers to perform basic surgical procedures and facilitate patient transfers. These clinical officers often do not have direct access to surgical specialists. As a result, cases outside their area of expertise are often referred to central hospitals without prior communication and with limited opportunities for receiving feedback on the patient’s subsequent treatment and care.
Birth of the WhatsApp consultation network
To fix this, a project called Scaling up Safe Surgery for District and Rural Populations in Africa (SURG Africa) initiated a remote Managed Network Consultation (MCN) in 2018 using WhatsApp. Chikwawa District Hospital and eight other district hospitals in southern Malawi gained real-time access to specialist advice and supervisory support. By leveraging WhatsApp, clinical officers and anaesthesia providers in district hospitals consult with surgeons and anaesthesiologists at Queen Elizabeth Central Hospital and Zomba Central Hospital, the region’s main referral centres.
According to Dr Jakub Gajewski, SURG Africa project leader, the initiative started with the aim of strengthening healthcare services and bridging the gap between rural and urban referral hospitals, ensuring equitable access to surgical expertise.

“In the beginning, SURG Africa sent surgeons from central hospitals to district hospitals once every month to train clinical officers, but then the question was what happens if the surgeons go back to the central hospitals?” said Gajewski. “The original idea was to create an app specially for consultations and enable them to share images and videos, but then it became so apparent that WhatsApp is widely used in Malawi, and there was no need to create another app.”
How it works
When the district team encounters a complex case, the clinical officer shares the case on the WhatsApp group platform seeking specialist guidance. The specialists provide recommendations for managing cases at the district level or they suggest necessary steps to be taken before referral. This collaborative approach enables rural clinicians and central hospital specialists to monitor the patient’s progress and maintain communication through the group forum. In addition, specialists can track the ongoing progress of cases treated at the district facility by following updates shared on the forum.
The project, which concluded in 2021, has evolved into a vital support system for rural hospitals facing clinical challenges. The WhatsApp group, now compromising about 400 medical personnel, has become an integral part of standard practice for all referrals to central hospitals. A study conducted in 2019 examined the usage of the WhatsApp group for specialist advice in district hospitals. The findings indicated that out of 249 surgical cases, 96% received advice through the group. Furthermore, 74% of cases received a response within an hour of posting, and in 68% of the cases, a decision was taken within an hour of posting the case on the group.

The WhatsApp group was also useful in reducing unnecessary referrals and saving costs for patients, guardians, referring hospitals, and the health system. According to the report, a potential referral cost of $ 5,580 per year for the nine district hospitals was saved.
Martin Malunga, a clinical associate at Mulanje District Hospital in southern Malawi, confirmed that the group has significantly enhanced the referral system in the country. “Before the WhatsApp group, clinicians only filled a referral form with clinical information, which was carried by the patient transferred to the central hospital, so if mismanagement had already happened at the district level, it was difficult for the specialists to deal with the problem,” he said adding “From Mulanje District Hospital, we post about two to three cases in a week.”
Dr Tiyamike Kapalamula, a paediatric surgeon at Queen Elizabeth Central Hospital who offers advice on the group, emphasises the positive impact. “We now receive patients in better condition because the necessary steps have already been taken at the district level since we are able to communicate instantly,” she said.
While recognising potential ethical concerns over sharing patient data on WhatsApp, strict guidelines apply to what content can be posted. To safeguard privacy, no patient names, faces or identifiable images are shared on the group.
Spillover benefits amidst challenges
Delays in receiving feedback do arise on occasion as a result of the overwhelming caseload at central hospitals, as well as high traffic in the Whatsapp group, which creates communication challenges.
Nonetheless, clinicians have been advised to repost cases during less busy periods to ensure prompt attention. Moreover, Malunga says “sometimes there are conflicting views from the specialists on a particular case until a consensus is reached.”
Since the consultation network was only introduced in central hospitals and rural hospitals in Southern Malawi, Gajewski reports that the central and rural hospitals in the northern and central parts of the country have started to create their own surgery WhatsApp groups without SURG Africa’s intervention.
“Because this is a no-cost thing, it just takes people’s willingness and time to set it up, and those in the central and northern part observed and realised that it is a doable tool, “said Gajewski. “Even for this initiative that we [SURG Africa] started in the southern region, different professions have created their own groups which have come out from the general group. For example, there’s one focusing on obstetrics and gynaecology; there’s another on anaesthesia and another for orthopaedics.”
With time, the network has provided other benefits, such as allowing the Ministry of Health to closely monitor surgical activities in the districts and to respond faster to shortages of essential surgical resources. According to Dr Jones Mwase, the deputy director of clinical services who is responsible for clinical practice in the Ministry of Health, “Surgery needs a lot of resources, and through this WhatsApp group, we have been able to respond and send over medical supplies such as surgical lamps and gloves and others. This direct link has enabled us to know what’s needed urgently.”
Mwase believes that technology is critical for strengthening basic healthcare delivery and expanding access to primary healthcare.
Although the SURG-Africa project ended in 2021, the MCN is growing and expanding. The MCN has embarked on a new initiative called kidSURG, which is dedicated to addressing paediatric patients’ surgical needs in rural Malawi. By targeting the specific needs of children, kidSURG aims to bridge the gap and provide essential surgical expertise in district hospitals, ensuring quality care.